Thyroid: Symptoms, Tests, Treatment, and Practical Tips
Thyroid problems are common and often easy to miss. This page gives clear, practical steps to spot thyroid issues, what tests matter, and how treatments work so you can ask the right questions at the clinic.
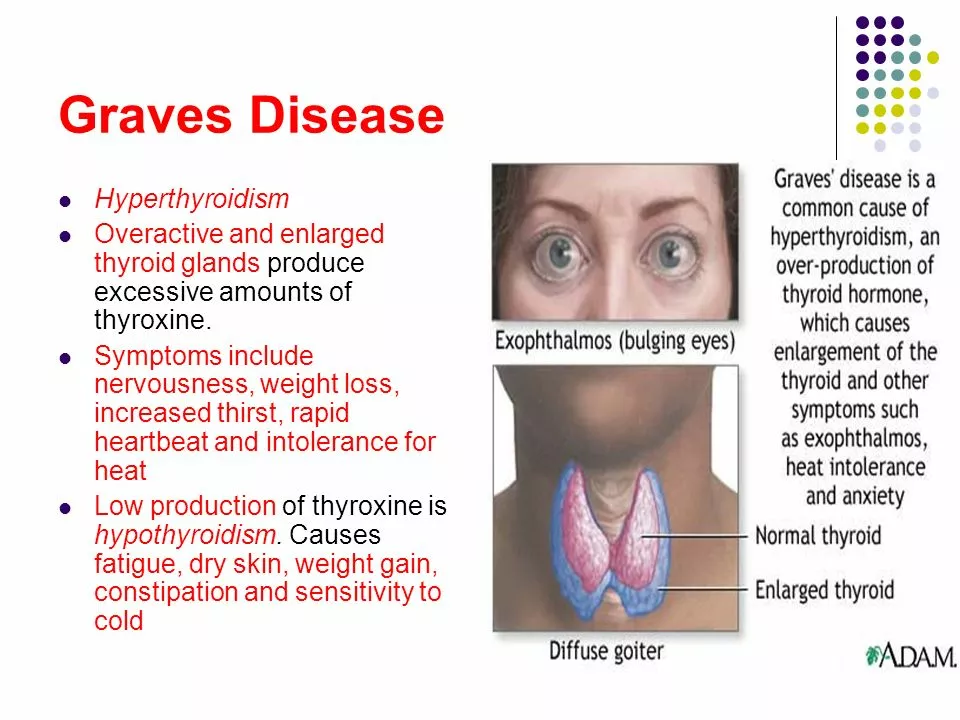
The thyroid is a small gland at the base of the neck that controls metabolism, energy, and body temperature. When it slows down (hypothyroidism) you might feel tired, cold, constipated, depressed, or gain weight without changing your diet. When it speeds up (hyperthyroidism) you can have palpitations, weight loss, sweating, anxiety, and tremors. Eye changes or a visible neck swelling may point to specific conditions like Graves' disease or a goitre.
Start with the right tests. Ask your doctor for TSH first. If TSH is abnormal, request free T4 and possibly free T3. If autoimmune disease is suspected, ask for thyroid peroxidase (TPO) and thyroglobulin antibodies. For suspected hyperthyroidism, a radioactive iodine uptake scan or thyroid ultrasound might be needed. Lab timing matters: if you take levothyroxine, hold it and test before your morning dose to get accurate levels.
If you have hypothyroidism, the usual treatment is levothyroxine. Take it on an empty stomach, 30-60 minutes before breakfast, or at bedtime at least four hours after the last meal. Avoid calcium, iron, aluminum, and some soy products within four hours of the pill - they lower absorption. Your doctor will adjust the dose based on TSH every 6-8 weeks until stable, then about once a year. Don't switch brands or formulations without checking your TSH sooner.
Hyperthyroidism treatments vary: antithyroid drugs (like methimazole), beta blockers for symptoms, radioactive iodine, or surgery in certain cases. Each option has trade-offs. Antithyroid drugs can cause side effects like rash or low white blood cell counts, so report new fevers or bruising immediately.
Special situations: pregnancy changes thyroid needs - women on levothyroxine usually need a higher dose and closer monitoring. Older adults and people with heart disease need careful dose changes to avoid angina or arrhythmia. Subclinical cases with mild lab changes may be watched rather than treated; discuss risks and benefits with your clinician.
Lifestyle helps but won't replace medication when levels are abnormal. Keep a balanced diet with adequate iodine if you live where deficiency is possible, avoid high-dose supplements unless advised, and aim for steady sleep, regular exercise, and stress control. Some trials show selenium supplements can reduce thyroid antibody levels in autoimmune thyroiditis, but ask your doctor before starting any supplement.
If you have new rapid heartbeat, severe weight change, high fever, or confusion, seek urgent care. For routine concerns, document symptoms, bring current medications and supplements, and ask for clear follow-up tests and targets. Our site covers medication safety, online pharmacy tips, and more guides to help you manage thyroid health confidently.
Before appointments, bring a checklist: symptoms with start dates, all medications and supplements, recent lab results, specific questions about side effects or fertility, and any pregnancy plans. A quick neck photo series can help track visible changes over time regularly.