It’s easy to think that if something is natural, it’s safe-especially when it comes to food or supplements. But the truth is, your morning grapefruit, your daily fish oil pill, or that herbal tea you drink for sleep could be quietly messing with your prescription meds. And you might not even know it.
Drug interactions happen when something you eat, drink, or take as a supplement changes how your medication works. It might make it weaker, stronger, or even cause dangerous side effects you didn’t sign up for. This isn’t rare. In fact, it’s one of the top five medication safety issues the World Health Organization warns about. And with nearly 4 in 10 Americans taking supplements, the risk is real-and growing.
How Interactions Work: Two Main Ways
Not all interactions are the same. They fall into two big categories: pharmacodynamic and pharmacokinetic.
Pharmacodynamic interactions happen when two substances affect your body in similar or opposite ways. For example, if you’re taking a blood thinner like warfarin and also take ginkgo biloba, both can thin your blood. Together, they might push your body into a bleeding risk zone. On the flip side, if you’re on blood pressure medication and take yohimbine (a supplement sometimes used for energy), the two can fight each other-making your BP meds useless.
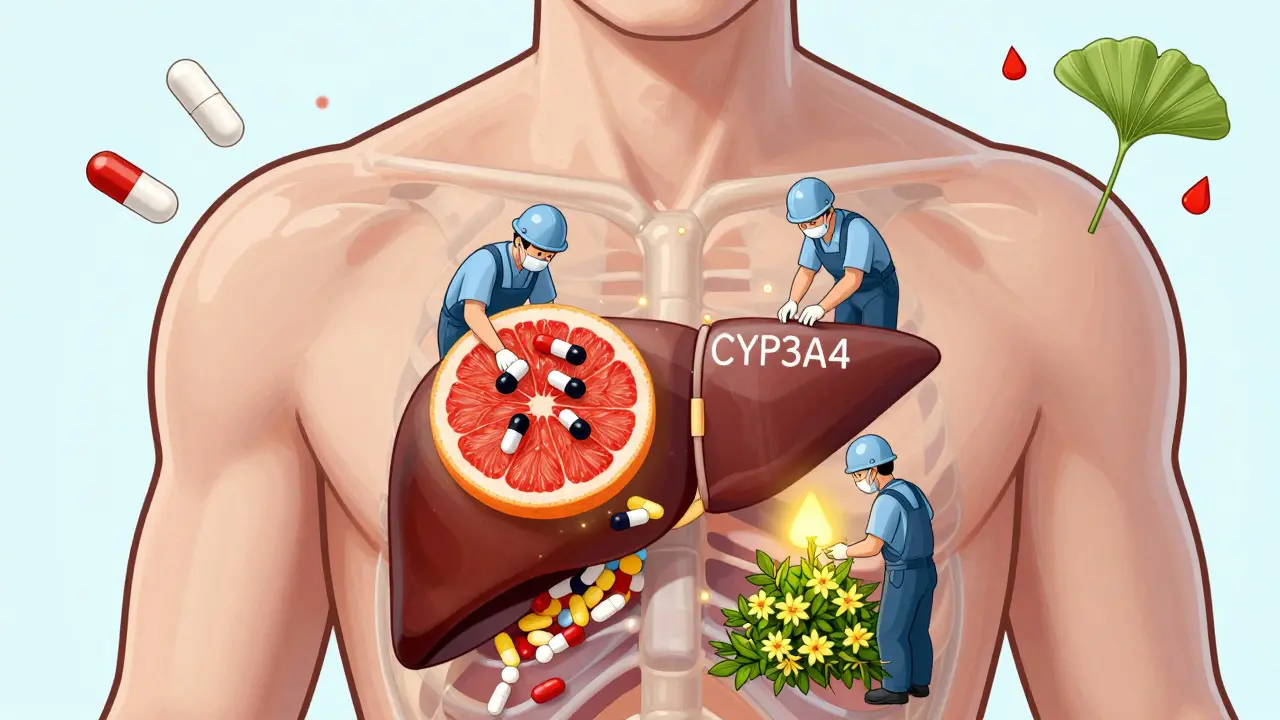
Pharmacokinetic interactions are sneakier. They change how your body absorbs, breaks down, or gets rid of a drug. Most of the time, this happens in the liver, thanks to a group of enzymes called cytochrome P450. These enzymes are like factory workers processing drugs. If something interferes with them-say, St. John’s wort-it can either slow things down (making the drug build up to toxic levels) or speed them up (making the drug disappear before it can work).
St. John’s wort is one of the worst offenders. It turns on the CYP3A4 enzyme like a switch. That enzyme breaks down about half of all prescription drugs. So if you’re on birth control, that pill might not work. If you’re on cyclosporine after a transplant, your body could reject the organ. If you’re on an SSRI for depression, you could develop serotonin syndrome-fever, muscle spasms, confusion, even death. And all because you took a “natural” herb for mood support.
Grapefruit: The Most Dangerous Fruit
Let’s talk about grapefruit. It’s healthy. It’s delicious. And if you’re on certain medications, it’s a ticking time bomb.
Grapefruit contains chemicals called furanocoumarins that permanently block the CYP3A4 enzyme in your gut. That means your body can’t break down the drug properly. The result? A huge spike in drug levels in your blood.
Take simvastatin, a common statin for cholesterol. Eating just one grapefruit can raise its levels by up to 15 times. That doesn’t just mean more side effects-it means a 10x higher risk of rhabdomyolysis, a condition where muscle tissue breaks down and clogs your kidneys. In one study, the rate jumped from 0.15 cases per 100,000 people a year to 1.57. That’s not a coincidence. It’s a direct effect.
And it’s not just grapefruit. Seville oranges, pomelos, and even some types of tangerines do the same thing. If your med label says “avoid grapefruit,” don’t assume it’s just a suggestion. It’s a warning backed by real data.
Supplements That Fight Your Meds
Supplements aren’t regulated like drugs. That means no one checks what’s in them before they hit shelves. And no one forces manufacturers to warn you about interactions.
Here are three of the most dangerous combos:
- St. John’s wort + antidepressants: As mentioned, it can trigger serotonin syndrome. It also cuts the effectiveness of HIV meds, birth control, and transplant drugs.
- Ginkgo biloba + blood thinners: Ginkgo prevents platelets from clumping. Warfarin, aspirin, clopidogrel-all do the same. Together? You’re looking at internal bleeding, stroke risk, or worse. Studies show it can increase bleeding time by 30-50%.
- Garlic supplements + anticoagulants: Over 30 case reports link garlic pills to uncontrolled bleeding in people on warfarin or heparin. Even high-dose garlic capsules can double your bleeding risk.
And don’t forget red yeast rice. It sounds harmless-“natural cholesterol reducer,” right? But it contains lovastatin, the same active ingredient in prescription statins. Taking it with a statin pill? You’re essentially doubling your dose. That increases muscle damage risk by more than double.

Food and Warfarin: A Delicate Balance
Warfarin is one of the most common drugs with food interactions. It’s used to prevent clots after strokes, heart attacks, or surgeries. But it’s also one of the most sensitive to diet.
Vitamin K is the key. It helps your blood clot. Warfarin works by blocking vitamin K. So if you suddenly eat a lot of vitamin K-rich foods-spinach, kale, broccoli, Brussels sprouts-your blood thickens. Your INR drops. You’re at risk for clots.
But here’s the twist: You don’t have to stop eating greens. You just have to keep them consistent. A 2018 study found that eating 150g of cooked spinach (830mcg of vitamin K) in one day dropped warfarin’s effect by 30-40%. But if you eat that same amount every day? Your body adjusts. Your INR stays stable.
The FDA recommends women aim for 90mcg of vitamin K daily, men for 120mcg. That’s about one cup of raw spinach. It’s not about avoiding food-it’s about routine.
And watch out for cranberry juice. It’s been linked to at least 28 cases of dangerous bleeding in warfarin users. INR levels spiked over 8.0-way above the safe range of 2.0-3.0. Even small amounts can do it.
What You Can Do: 5 Practical Steps
You don’t need to quit supplements or stop eating healthy foods. But you do need to be smart.
- Make a complete list. Write down every pill, capsule, tea, powder, or tincture you take-even the ones you think are “just for fun.” Include OTC meds like ibuprofen or antacids. Update it every time you see a doctor.
- Ask your pharmacist. They’re trained to spot interactions. When you pick up a new prescription, ask: “Could this interact with anything I’m already taking?”
- Use free tools. The FDA’s Drug Interaction Checker and MedlinePlus’s tool let you type in your meds and supplements. They’ll flag high-risk combos.
- Don’t start new supplements without asking. Just because your friend swears by turmeric for arthritis doesn’t mean it’s safe for you. Talk to your doctor first.
- Keep a food log if you’re on warfarin. Note how much leafy green you eat each week. Share it with your provider. Consistency is your friend.
Why This Matters More Than You Think
These aren’t just theoretical risks. Between 2013 and 2019, 23% of serious adverse events tied to supplements were due to drug interactions. That’s not a glitch. It’s a pattern.
And here’s the kicker: 70% of people don’t tell their doctors they’re taking supplements. Why? They think it’s not “real medicine.” But your doctor needs to know. Because even a “safe” herb can turn deadly when mixed with your heart meds or blood pressure pills.
Pharmacists estimate that medication reviews that include supplements reduce adverse events by 22%. That means fewer hospital visits, fewer emergencies, and lower costs. One study found that pharmacist-led care saved $1,123 per patient per year.
And the system is catching up. The FDA now requires new drugs to be tested for interactions with common supplements. AI tools are being trained to predict hidden risks by scanning millions of medical notes. But none of that matters if you don’t speak up.
Final Thought
You’re not being paranoid. You’re being careful. Medications are powerful. So are supplements. So is food. When they meet, things can go wrong fast. But they don’t have to. The answer isn’t to stop taking what helps you. It’s to talk about it. To ask questions. To be informed.
Because the safest medicine is the one you understand.
Can I still eat grapefruit if I’m not on medication?
Yes. Grapefruit is perfectly safe if you’re not taking any medications that interact with it. The risk only exists when you combine it with certain drugs-like statins, blood pressure meds, or immunosuppressants. If you’re unsure, check your med list or ask your pharmacist.
Are all supplements risky?
No. Many supplements are safe when used correctly. The problem isn’t the supplement itself-it’s the combination. For example, vitamin D, calcium, and magnesium are generally low-risk. But herbs like St. John’s wort, ginkgo, and garlic have well-documented interaction profiles. Always research or ask before adding anything new.
What if I take a supplement that’s not on the list?
Just because it’s not in a database doesn’t mean it’s safe. Many supplements aren’t studied well enough to be listed. The safest approach is to assume any supplement could interact-especially if you’re on a prescription drug. Always disclose everything to your doctor or pharmacist.
Can I take supplements at a different time than my meds?
Sometimes, spacing them out helps-but not always. For example, St. John’s wort changes how your liver works for days, even weeks. Taking it 2 hours apart won’t fix that. With grapefruit, even a single serving can block enzymes for 24 hours. Timing matters for some interactions, but not all. The best rule: talk to your provider before changing anything.
Do over-the-counter drugs interact too?
Absolutely. Even simple painkillers like ibuprofen or naproxen can increase bleeding risk when taken with blood thinners. Antacids can reduce absorption of antibiotics or thyroid meds. Don’t assume OTC means safe. Always check interactions, even for non-prescription items.


8 Comments
Tobias Mösl
So let me get this straight-you’re telling me my daily grapefruit smoothie is basically a slow-motion suicide pact if I’m on statins? And nobody told me this until now?
My cousin died from rhabdomyolysis after ‘just eating half a grapefruit’ while on simvastatin. The hospital said it was ‘unexplained.’ Unexplained?! It was right there on the bottle.
Pharmaceutical companies don’t want you to know this. Supplements? ‘Natural’ my ass. They’re not regulated because they’re not profitable enough to test. But when they kill people? Oh, now it’s a ‘public health issue.’
I’ve been tracking every drug I take with a spreadsheet. St. John’s wort? Deleted. Garlic pills? Gone. Even my omega-3s are now timed 4 hours apart from my blood pressure med. I don’t trust anyone. Not my doctor. Not the FDA. Not the ‘wellness influencers’ who sell you ‘immune boosters’ while sipping their grapefruit kombucha.
They’re all just waiting for you to die so they can sell you the next miracle cure.
Mariah Carle
I just... I don't know anymore. 😔
I took turmeric for my knees. Then I started on lisinopril. Now I'm scared to move. What if I'm silently bleeding inside? What if I'm just one banana away from a stroke?
My grandma used to say, 'If it doesn't come from a pharmacy, it doesn't belong in your body.' I thought she was old-fashioned. Now I think she was a prophet.
I deleted all my supplement apps. I'm just... eating food. Plain food. And praying.
Justin Rodriguez
I work as a clinical pharmacist and this post is spot-on. The real tragedy isn’t the interactions-it’s how rarely patients disclose supplements.
I had a 68-year-old man last week who was on warfarin and taking ‘a little garlic’ for his cholesterol. He didn’t think it counted. His INR was 8.2. He nearly bled out.
Here’s the thing: It’s not about fear. It’s about awareness. You don’t need to quit everything. You just need to talk. Bring your pill bottle. List every tea, powder, and tincture-even the ones you think are ‘harmless.’
And yes, grapefruit is dangerous. But so is OTC melatonin with antidepressants. So is St. John’s wort with birth control. We’re not scared of natural things. We’re scared of silence.
Megan Nayak
Oh, so now we’re all supposed to be terrified of food?
Let me guess-next they’ll tell us oxygen interacts with aspirin.
Look, if you’re on warfarin and you eat kale, your INR drops. If you eat spinach, it drops. If you eat... nothing? It goes up. So what’s the solution? Eat the same damn greens every day. Not ‘avoid’ them. Not ‘panic.’ Just be consistent.
And St. John’s wort? Maybe it’s not the herb. Maybe it’s the fact that people take 1000mg of unregulated junk from a guy named ‘HerbalBob’ on Amazon.
Blaming grapefruit? Blaming supplements? This is like blaming a hammer because someone used it to break a window. The problem isn’t the tool. It’s the idiot holding it.
Sharon Lammas
There’s a deeper truth here, I think.
We’ve been taught that medicine is magic. That a pill can fix anything. And that ‘natural’ means pure. But biology doesn’t care about our labels.
Every substance-whether synthesized in a lab or grown in soil-interacts with our bodies through the same channels. The liver doesn’t know if a compound came from a pharmacy or a farmer’s market.
So maybe the real issue isn’t grapefruit or ginkgo. It’s our refusal to see ourselves as complex, fragile systems. We want simple answers: ‘Take this, avoid that.’ But the truth is messier.
We need humility. Not fear. We need curiosity-not paranoia.
marjorie arsenault
You got this. Seriously.
Start small. Write down one thing you take every day. Just one. Then ask your pharmacist. That’s it.
One step. One conversation. One less thing to worry about tomorrow.
You’re not alone. And you don’t have to do it all today. Just one thing. You’re doing great.
Deborah Dennis
So... you’re saying I can’t have my grapefruit? My fish oil? My ‘natural’ sleep aid? And I have to ask my doctor? And my pharmacist? And look up interactions? And keep a log? And what if I forget? And what if they’re wrong? And what if I die anyway?
...I’m just gonna stop taking everything. Except coffee. And wine. And my Tylenol. And my melatonin. And my magnesium. And my protein powder. And my vitamin D. And...
Wait. I’m doomed.
Diane Croft
I used to think supplements were harmless. Then my mom had a stroke because she took ginkgo with her blood thinner. She’s fine now. But she’ll never take another pill without checking first.
So I started asking. Every time. Even for ibuprofen.
It’s not scary. It’s just... responsible.
And honestly? My doctor appreciates it. She says I’m one of the few patients who actually shows up prepared.
You’re not overthinking. You’re being smart.