Open-Angle Glaucoma: What to Watch For and What To Do
Glaucoma can steal vision slowly and quietly. Open-angle glaucoma is the most common type. You may not notice it until significant vision is lost. That’s why knowing the signs, tests, and simple steps to slow progression really matters.
What is open-angle glaucoma?
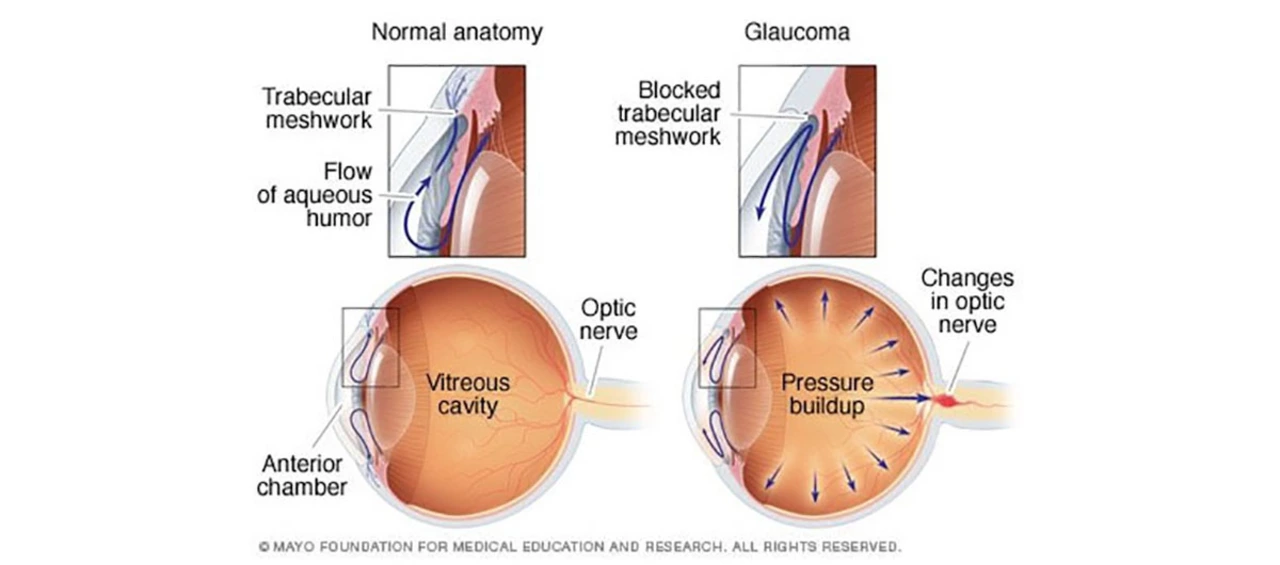
Open-angle glaucoma happens when fluid drains too slowly from the eye. That raises pressure inside the eye (intraocular pressure). Over time higher pressure damages the optic nerve, which carries visual information to your brain. The term “open-angle” refers to the angle where drainage occurs — it stays open, but the drainage tissues don’t work well.
Risk factors include age (over 60), family history, African or Hispanic ancestry, high eye pressure, thin corneas, and some medical conditions like diabetes. Many people have no pain or early symptoms, so regular eye checks are the only reliable way to catch it early.
How is open-angle glaucoma spotted and treated?
Eye doctors use a few quick tests. Tonometry measures eye pressure. Ophthalmoscopy checks the optic nerve for signs of damage. Visual field tests reveal blind spots you might not notice. Optical coherence tomography (OCT) images the nerve and retina for early changes. If tests show a problem, your doctor will recommend treatment to lower eye pressure and protect vision.
First-line treatment is usually daily eye drops. Common classes: prostaglandin analogs (often once a day), beta-blockers, carbonic anhydrase inhibitors, alpha agonists, and Rho kinase inhibitors. Each works differently. Side effects vary, so tell your doctor about allergies and other medicines you take.
If drops aren’t enough, laser trabeculoplasty can improve drainage and reduce pressure for months or years. For more severe cases, surgeries like trabeculectomy or minimally invasive glaucoma surgeries (MIGS) create new pathways for fluid to leave the eye. Your eye surgeon will explain risks and recovery times.
Practical tips: take your drops exactly as prescribed — missing doses raises risk of vision loss. Use reminders or a pillbox for eye drops. Bring a list of all your meds to the eye clinic. Ask about generic options and patient assistance if cost is an issue. Keep follow-up visits — glaucoma is a long-term condition that needs monitoring.
Watch for sudden symptoms like eye pain, nausea, blurred vision, or rainbow halos around lights — those are emergency signs and need urgent care. Otherwise, focus on consistent care: regular screenings, medication adherence, and lifestyle habits such as controlling blood pressure and not smoking.
If someone in your family has glaucoma, tell your eye doctor and schedule regular checks earlier. Catching open-angle glaucoma early gives you the best chance to keep your sight for years to come.