Opioid Overdose Response Assistant
Is This an Opioid Overdose?
This interactive tool helps you quickly identify opioid overdose signs and provides immediate guidance for emergency response. Every second counts.
Emergency Response Guide
Please complete the assessment above to receive guidance.
When someone overdoses on opioids, time isn’t just important-it’s the only thing standing between life and death. Breathing stops. Oxygen cuts off. Brain cells begin dying within minutes. And yet, most people don’t know what to look for or what to do. This isn’t a rare event. In the U.S., over 180 people die every day from drug overdoses, and nearly 8 out of 10 of those involve opioids. Fentanyl, a synthetic opioid 50 to 100 times stronger than morphine, is now mixed into pills, powders, and even fake Xanax. You might not even know you’re handling something deadly. But if you can recognize the signs and act fast, you can save a life.
What Happens During an Opioid Overdose?
Opioids-whether prescription painkillers like oxycodone, heroin, or illicit fentanyl-work by attaching to receptors in the brain that control breathing. When too much of the drug floods the system, it shuts down those signals. The person stops breathing. Their body doesn’t get oxygen. Their heart slows. Their skin turns blue or gray. Within 4 to 6 minutes, brain damage starts. Without help, death follows soon after.
This isn’t just about people who use drugs illegally. Many overdoses happen to people taking prescribed opioids for chronic pain. Others mix opioids with alcohol or benzodiazepines, which makes breathing suppression worse. And because fentanyl is so potent, even a tiny amount can be fatal. A pill that looks like a regular painkiller might contain enough fentanyl to kill someone who’s never used opioids before.
The Three Key Signs of an Opioid Overdose
If you suspect someone is overdosing, look for these three core signs-the classic triad doctors use to confirm opioid poisoning:
- Unresponsive-Try shaking their shoulders and shouting their name. No reaction? That’s a red flag.
- Slow, shallow, or stopped breathing-Watch their chest. Are they taking fewer than 8 breaths per minute? Or is there no movement at all?
- Pinpoint pupils-Their pupils should be tiny, like pinpricks, even in dim light. (Note: Not everyone shows this, so don’t wait for it.)
Other warning signs include:
- Blue, purple, or gray lips and fingernails
- Cold, clammy skin
- Gurgling, choking, or snoring sounds (this is the body struggling to breathe)
- Limp body, like a ragdoll
- Extreme drowsiness or inability to stay awake
Don’t wait for all the signs. If someone is unresponsive and breathing poorly, assume it’s an overdose. Every second counts.
What to Do in an Emergency: The 3-Step Response
The best thing you can do? Follow this simple, life-saving protocol endorsed by the CDC, Health Canada, and emergency medical services worldwide:
- Call 9-1-1-Right away. Even if you’re not sure. Tell them it’s a possible opioid overdose. Emergency responders will prioritize this call.
- Give naloxone-If you have it, use it now. Naloxone (brand name Narcan) is a nasal spray that reverses opioid effects in minutes. No prescription is needed in most places. It’s safe-even if they didn’t take opioids, it won’t hurt them.
- Stay with them until help arrives-Naloxone wears off in 30 to 90 minutes. The opioids might still be in their system. They could stop breathing again. Keep checking their breathing. If they stop, start CPR.
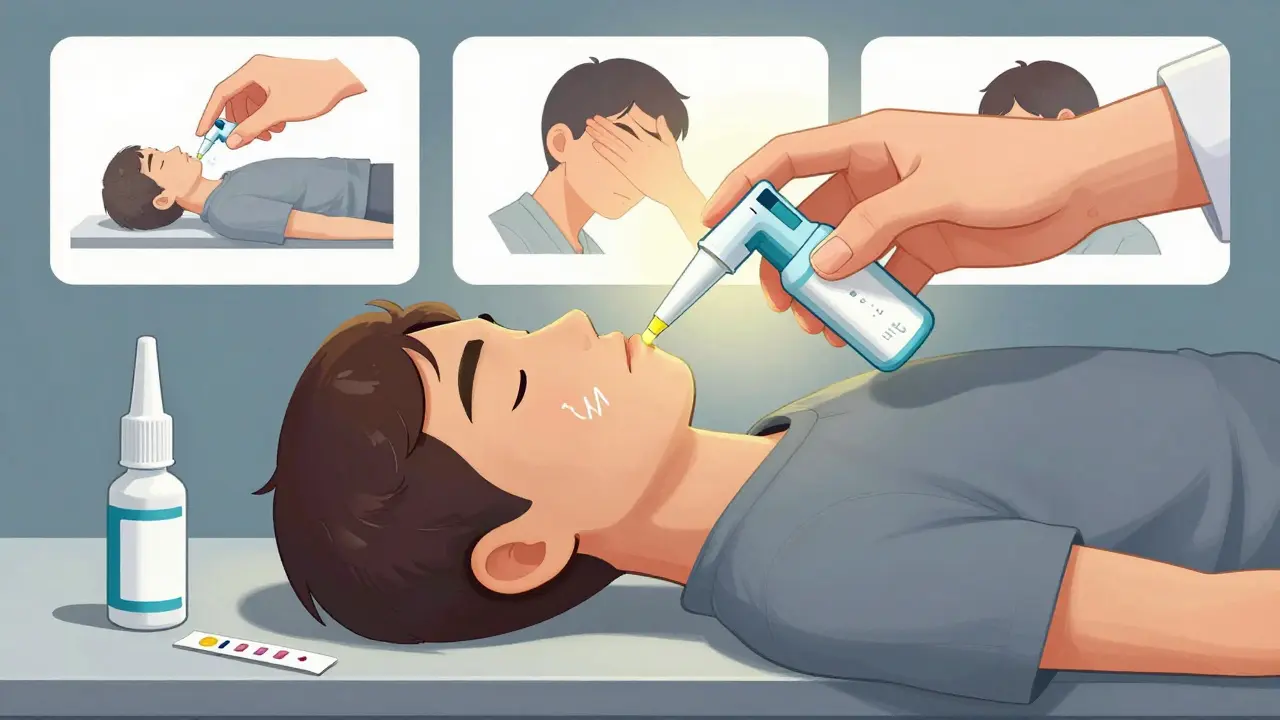
Here’s how to use naloxone nasal spray:
- Remove the spray from its package.
- Hold it with your thumb on the bottom and your fingers on either side.
- Tilt the person’s head back slightly.
- Insert the nozzle into one nostril.
- Press the plunger firmly to deliver the full dose.
- Turn them onto their side (recovery position) to keep their airway open.
- Wait 2 to 5 minutes. If no response, give a second dose in the other nostril.
Many pharmacies now give out naloxone for free or at low cost. Some states allow pharmacists to hand it out without a prescription. Keep one at home, in your car, or with your wallet. It’s small. It’s cheap. It could save someone’s life.
Why Naloxone Works-and Why It’s Not a Cure
Naloxone doesn’t treat addiction. It doesn’t fix the problem. It just buys time. It works by kicking opioids off the brain’s receptors, letting breathing restart. But it doesn’t last long. Fentanyl, in particular, sticks around longer than naloxone. That’s why people can die after being revived-because the overdose comes back.
That’s why staying with the person is critical. Even if they wake up, they need medical care. Their body may still be under stress. Their organs may be damaged. They need to be checked for heart problems, lung injury, or brain swelling.
And here’s something important: naloxone has zero effect on non-opioid drugs like cocaine, meth, or alcohol. But if you’re unsure what someone took, give naloxone anyway. It won’t harm them. And if they did take opioids, it could be the difference between life and death.
Real-World Impact: How Communities Are Saving Lives
Communities that train people to use naloxone have seen overdose deaths drop by up to 14%. In Virginia, the REVIVE! program has trained over 150,000 people-including police officers, baristas, and parents-to respond to overdoses. In Australia, naloxone is now available over the counter in pharmacies without a prescription.
Fentanyl test strips are another tool gaining traction. For less than $1, you can test a small sample of powder or a crushed pill to see if fentanyl is present. It’s not perfect, but it’s better than guessing. Some harm reduction centers hand them out with naloxone kits.
And while naloxone saves lives, it’s only part of the solution. After an overdose, the person needs medical follow-up, mental health support, and access to treatment. Many overdose survivors don’t get that help. That’s why it’s crucial to connect them with resources-not just to revive them, but to help them survive the next day, the next week, the next year.
What You Can Do Today
You don’t need to be a doctor to make a difference. Here’s what you can do right now:
- Get a naloxone kit-Visit your local pharmacy. Ask for it. You don’t need a prescription.
- Learn how to use it-Watch a 2-minute video from the CDC or Health Canada. Practice on a dummy spray.
- Keep one handy-In your purse, glove compartment, or first aid kit.
- Talk about it-Tell friends, family, coworkers. Break the silence. Overdoses happen in quiet homes, not just alleyways.
- Know the signs-If someone looks unresponsive and their breathing is off, act. Don’t wait for a label.
Every overdose is preventable. Not because we can stop addiction overnight. But because we now have a tool that works-when used in time. And that tool is in your hands.
Can naloxone hurt someone who didn’t take opioids?
No. Naloxone only works on opioid receptors. If someone hasn’t taken opioids, it won’t have any effect on them. It won’t cause harm, trigger withdrawal, or make them sick. If you’re unsure whether opioids were involved, give naloxone anyway. The risk of doing nothing is far greater.
How long does naloxone last, and why do people need more than one dose?
Naloxone typically lasts 30 to 90 minutes. But many opioids, especially fentanyl, last much longer. This means the overdose can return after the naloxone wears off. That’s why giving a second dose-and staying with the person-is essential. Emergency responders always carry extra doses for this reason.
Can you overdose on naloxone?
No. There is no known overdose limit for naloxone. It’s safe to give multiple doses if needed. In fact, if the person doesn’t respond to the first dose, giving a second one is standard practice. The only side effect might be sudden opioid withdrawal symptoms-like nausea, vomiting, or agitation-but these are not life-threatening.
Where can I get naloxone for free or cheap?
In Australia, naloxone is available over the counter at pharmacies for around $10-$20. In the U.S., many states offer free naloxone through public health programs, needle exchanges, or community organizations. Some pharmacies offer it at $0 with insurance. Check with your local health department or visit websites like naloxoneone.org for local options.
What should I do after reviving someone?
Even if they wake up, they still need medical care. Call 9-1-1 and stay with them. Their breathing could stop again. Once they’re stable, encourage them to see a doctor. Overdoses can cause internal damage that isn’t obvious. Long-term, they should consider counseling, medication-assisted treatment, or support groups. Recovery starts with connection-not judgment.






12 Comments
Paul Ratliff
i had a friend OD last year. didn't know what to do. just screamed. thank god a bouncer had naloxone. saved his life. now i carry two in my pocket. no joke. it's like a seatbelt for your heart.
SNEHA GUPTA
The human body is a fragile system governed by biochemical equilibrium. When exogenous opioids disrupt the endogenous opioid receptor dynamics, the respiratory center in the medulla oblongata is suppressed. This is not merely a pharmacological event-it is a metaphysical threshold between consciousness and oblivion. Naloxone, as a competitive antagonist, restores homeostasis. But the deeper question remains: why do we allow such suffering to become normalized?
Gaurav Kumar
In India we don't have this problem. Why? Because we have discipline. We don't let weak-minded people import American drug culture. Fentanyl is a Western disease. Your government lets corporations sell painkillers like candy. Then you wonder why people die. We don't need naloxone. We need moral clarity. 🇮🇳
David Robinson
Look. I get that this is supposed to be a life-saving guide. But let's be real. Most people who OD are just making bad choices. You can't save someone who doesn't want to be saved. And now we're handing out free narcan like candy? What's next? Free meth? This isn't prevention. It's enabling. And don't get me started on how many times these people OD again after being revived. It's a loop. A broken one. And taxpayers are footing the bill. I'm not heartless. I'm just tired of the charade.
gemeika hernandez
i had a cousin who OD'd. she was on oxycodone for back pain. never touched heroin. just took too much. they revived her. she didn't even remember. now she's in rehab. i keep a naloxone in my purse. just in case. you never know.
Nicole Blain
this made me cry 😭 i keep a naloxone in my glovebox now. my little sister’s boyfriend almost died last month. we were so scared. thank you for making this so clear. 💙
Kathy Underhill
The critical window for intervention is less than six minutes. Delaying emergency response to verify symptoms increases mortality. Naloxone administration is low-risk, high-reward. The emphasis should be on accessibility and education, not stigma. Medical follow-up is non-negotiable. Survival is not recovery.
Stephen Habegger
You don't need to be a hero. Just be prepared. One spray. One minute. One life. It's that simple. Keep one. Teach someone. Pass it on.
Justin Archuletta
I got mine from the pharmacy last week. No prescription. $0. They gave me a demo spray. I practiced on my cat. (She’s fine. She’s a cat.) I keep it next to my toothbrush. You never know when you’ll need it. Don’t wait. Just get it.
cara s
It is of paramount importance to recognize that the administration of naloxone, while efficacious in reversing opioid-induced respiratory depression, does not address the underlying psychosocial determinants of substance use disorder. Structural factors-including inadequate mental health infrastructure, economic disenfranchisement, and the pharmaceutical industry’s predatory marketing practices-must be confronted with systemic policy reform. The current paradigm of harm reduction, while laudable, remains a palliative measure within a failing system.
Amadi Kenneth
This is all a lie. Naloxone? It's a government tool to keep addicts alive so they can be tracked. The CDC doesn't care about you. They want to control populations. Fentanyl? It's not in the pills. The pills are clean. It's the 5G towers that are making people OD. You think you're saving lives? You're being used. Check the numbers. They don't add up.
Robin Hall
The assertion that naloxone is harmless in non-opioid cases is scientifically accurate. However, the widespread distribution of this agent without concurrent implementation of mandatory psychological screening or follow-up protocols constitutes a form of institutionalized negligence. The absence of regulatory oversight in the distribution chain raises serious ethical and epidemiological concerns. We are not saving lives; we are delaying inevitable systemic collapse.