Skin and Dermatology: Practical Care, Dermatitis Treatments & When to Seek Help
Got a stubborn rash or dry, itchy skin? You don’t always need heavy steroids. This page gives clear, practical tips on what works, what to try next, and when to see a dermatologist.
Steroid-sparing options for dermatitis
If you’re worried about long-term steroid use, two common non-steroid options are topical calcineurin inhibitors (like tacrolimus, pimecrolimus) and PDE4 inhibitors (like crisaborole). They calm inflammation without the skin-thinning risk of steroids. Expect some initial burning or stinging for a few days; that’s common and usually fades.
Use these meds exactly as your dermatologist tells you—often twice daily on affected areas until the flare eases, then less often to maintain control. They work well for face and neck where steroid thinning is a real concern. For mild flares, crisaborole can be a good first step; for more persistent or sensitive-area disease, calcineurin inhibitors often help.
Remember: creams and ointments deliver medicine differently. Ointments trap moisture and work best on very dry skin; creams feel lighter and absorb faster. Match the vehicle to where and how your skin reacts.
Everyday skin care that helps heal and prevent flare-ups
Start with a gentle routine. Cleanse with a mild, pH-friendly wash and lukewarm water. Hot showers strip oils and worsen dryness. Pat skin dry—don’t rub—and apply a thick moisturizer while skin is still damp to lock in moisture.
Pick fragrance-free products with ceramides or hyaluronic acid. For eczema-prone skin, thicker ointments at night and lighter lotions in the day work well. Use sunscreen daily—broad-spectrum SPF 30 or higher—especially if you’re on treatments that increase sun sensitivity.
Short-term steroid use is fine for many people, but avoid long-term high-potency steroids on the face, groin, or underarms. If you’re switching to a non-steroid option and symptoms worsen, call your provider for a plan that might combine treatments safely.
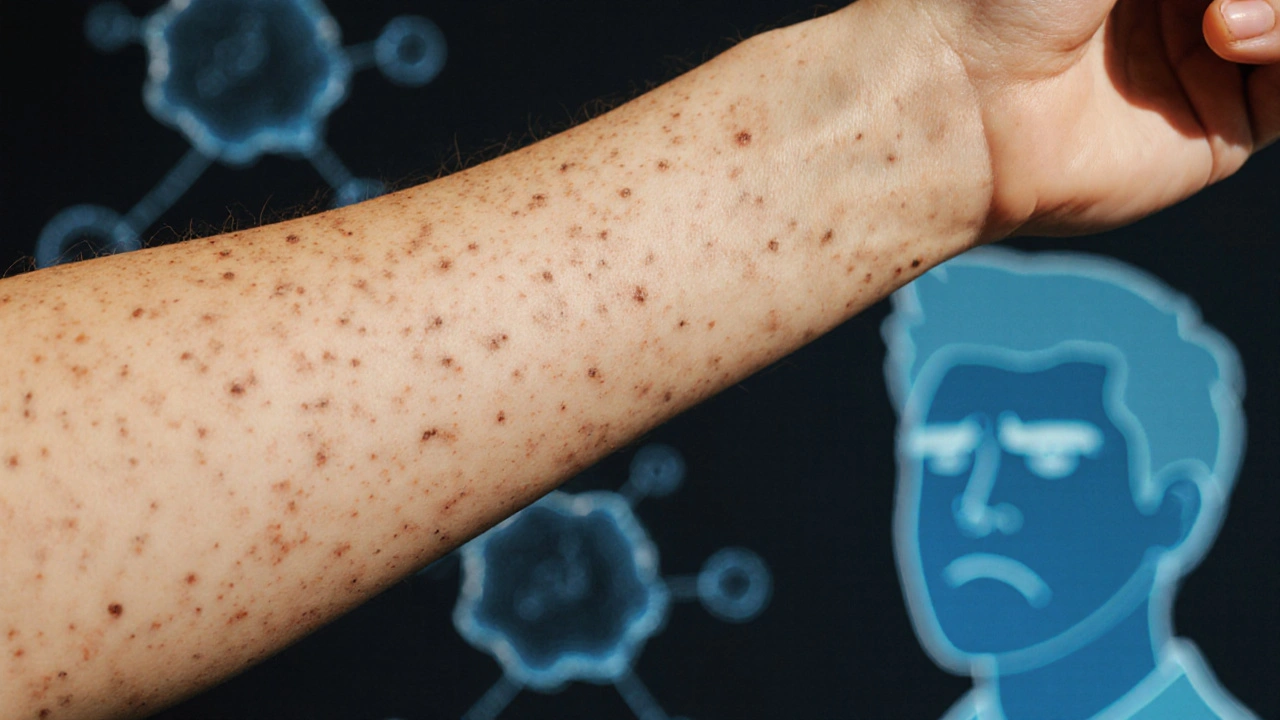
Now about rare conditions: if a patch of skin keeps changing, won’t clear with usual therapy, or looks different from your normal eczema, get it checked.
Mycosis fungoides can start as persistent, scaly patches that look like eczema or psoriasis but don’t respond to standard care. If a patch remains for months, grows, or you notice new lumps or swollen lymph nodes, ask a dermatologist about a skin biopsy and specialty testing. Early diagnosis changes the treatment path and helps you find the right specialist care.
Finally, keep a simple log: note what triggers flares (weather, stress, new soaps), what helped, and how long treatments took to work. That record makes appointments more productive and helps your clinician pick the best next steps.
If you want, read our deeper guides on steroid-sparing drugs and mycosis fungoides for more specifics on dosing, side effects, and real-world tips from patients and dermatologists.