Vision and Eye Health: Practical Tips for Better Eyes
Healthy vision affects work, hobbies, and safety every day. You can protect your eyes with simple habits and regular checks. This page collects clear, practical advice on common problems like dry eye, glaucoma, and general eye strain. Read on to learn what to watch for, what to ask your doctor, and easy steps you can try at home.
Dry eye feels like grittiness, burning, or blurred vision. It can come from weather, screen time, aging, or medications. Many people with open-angle glaucoma report dry eye symptoms too. Long-term use of topical glaucoma drugs, especially prostaglandin analogs, can worsen tear film stability for some patients. If you have both conditions, tell your eye doctor so they can adjust treatment or recommend lubricating drops.
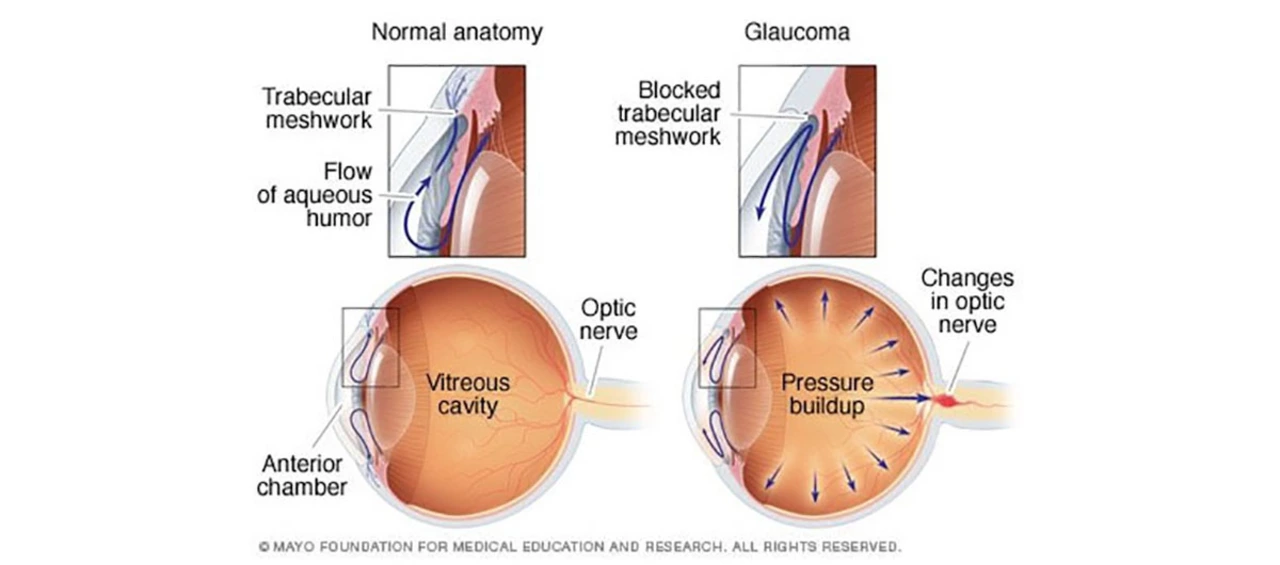
Open-angle glaucoma often has no pain and slowly reduces side vision. Regular eye exams with optic nerve checks and pressure tests catch glaucoma earlier. Visual field testing helps track changes over time. If you have risk factors — family history, high eye pressure, or certain ethnic backgrounds — get checked more often.
Simple daily habits cut symptoms and protect vision. Follow the 20-20-20 rule: every 20 minutes look 20 feet away for 20 seconds. Blink frequently during long screen sessions and position screens slightly below eye level. Use humidifiers in dry rooms and wear sunglasses that block UV rays outdoors. For contact lens wearers, follow cleaning and replacement guidelines to avoid irritation or infection.
When to see an eye care professional? Book an appointment if you notice sudden vision changes, flashes of light, new floaters, severe pain, or persistent redness. For chronic dryness that does not improve with over-the-counter drops, an evaluation can reveal underlying causes like meibomian gland dysfunction or allergy. If you suspect glaucoma, a comprehensive exam with imaging and pressure checks is the right step.
Treatment options are specific. Dry eye responds to artificial tears, eyelid hygiene, warm compresses, and sometimes prescription anti-inflammatory drops. For glaucoma, doctors use prescription eye drops, laser therapy, or surgery to lower eye pressure and slow damage. If medications cause severe dry eye, your doctor might switch drugs, change dosage, or add supportive therapies.
Nutrition, sleep, and exercise matter too. Eat foods rich in omega-3s, leafy greens, and colorful vegetables. Stay hydrated and sleep enough to help tear production and eye recovery. Moderate exercise improves circulation, which supports eye health.
Keep a record of symptoms, medications, and eye exam dates. That helps your doctor spot patterns and adjust care quickly. Minor changes at home can reduce discomfort and preserve vision. If you have questions about a specific eye condition or treatment, bring them up at your next visit.
Quick FAQs
Can eye drops for glaucoma cause dry eye? Sometimes yes, especially with long-term prostaglandin use. Talk to your doctor about alternatives or tear supplements. How often should you get checked? Most adults need a full eye exam every one to two years, sooner if you have risk factors or symptoms. Report new issues right away.